The Silent Culprit in Diabetes: How Fat Can Wreck Blood Sugar and Insulin Sensitivity
I’ve lived with type 1 diabetes for over 30 years. I’m also a Certified Diabetes Educator, a Registered Dietitian, and an author, so I love learning about food and how it impacts blood sugar. Diabetes has a way of teaching us lessons every day, and I continue to learn. What I learn, I share with others so we can all live healthier and happier lives with diabetes.
Before we jump in, some people do very well eating a high-fat diet, such as a keto or adapted keto approach. This article is for people who typically eat a higher-carb diet and have found high-fat, high-carb combinations challenging.
In the diabetes world, carbohydrates get most of the attention. We talk about carb counting, carb-to-insulin ratios, carb impact, carb timing, carb quality, and even carb fear. Protein gets some attention too, but the macronutrient that is most often overlooked is fat. Fat, especially saturated fat, is a silent and powerful player that can disrupt blood sugar management and insulin sensitivity if we do not pay attention.
The Day I Learned About Fat-Induced Insulin Resistance
The other day, I had a vivid reminder of this. I experienced a severe insulin resistance reaction that was not caused by a faulty infusion set, which is always my first guess when blood sugars go haywire. To triple-check that it was not the embedded cannula, which is not always visible since it is hidden under the skin, I left my current infusion set in. I normally tell people, “when in doubt, change it out,” but I did not. I wanted to experiment.
After that day, which was a truly terrible rollercoaster of blood sugar highs and lows, I kept the infusion set in and ate a moderate to low-fat diet. In theory, the infusion set was now a day older, so my numbers should have been worse if the issue was the infusion site. But even with the older set, my time in range increased by thirty percent. I avoided dangerous insulin stacking and the extreme blood sugar drops that made the previous day so terrifying.

What Happened That Day
On my day of 72% time in range, I had an extremely high intake of fat, including a lot of saturated fat, throughout the day. At dinner, I ate a carbohydrate-containing meal. My blood sugar stayed elevated for more than six hours, despite taking insulin for the carbohydrates.
As an educator, I can recognize this metabolic pattern almost immediately. You eat a high-fat, high-carb dinner. The effect is amplified if the fat is saturated and the carbohydrates are highly refined. The first hour looks fine. Everything seems under control. But ninety minutes in, the glucose begins to climb. First, it is just a slight upward arrow. Then it continues to climb until you are facing two arrows up. You are now tumbling into insulin resistance.
You bolus. Then you bolus again. Then your pump alerts that you have reached your maximum correction based on insulin on board. You start entering “fake carbs” just to bypass the pump’s limit. Your frustration rises. You wonder if your infusion set is bad. Is your insulin expired? Are you imagining things?
Hours pass. You are exhausted but scared. You want to sleep, but your continuous glucose monitor is screaming, and your insulin is stacked. Eventually, six to eight hours later, the blood sugar comes down. Often dramatically. On that day, it was like an avalanche. I was in deep REM sleep and awoke in a sweat, adrenaline through the roof. I grabbed not one, but two packs of Smarties, stuffed them in my mouth, and stayed alert and terrified.
It was terrifying. I did not want to repeat that experience. Using the same infusion set to test that the site was not the issue, I decided to look closely at what had caused it, understand the physiology, and adjust my approach.
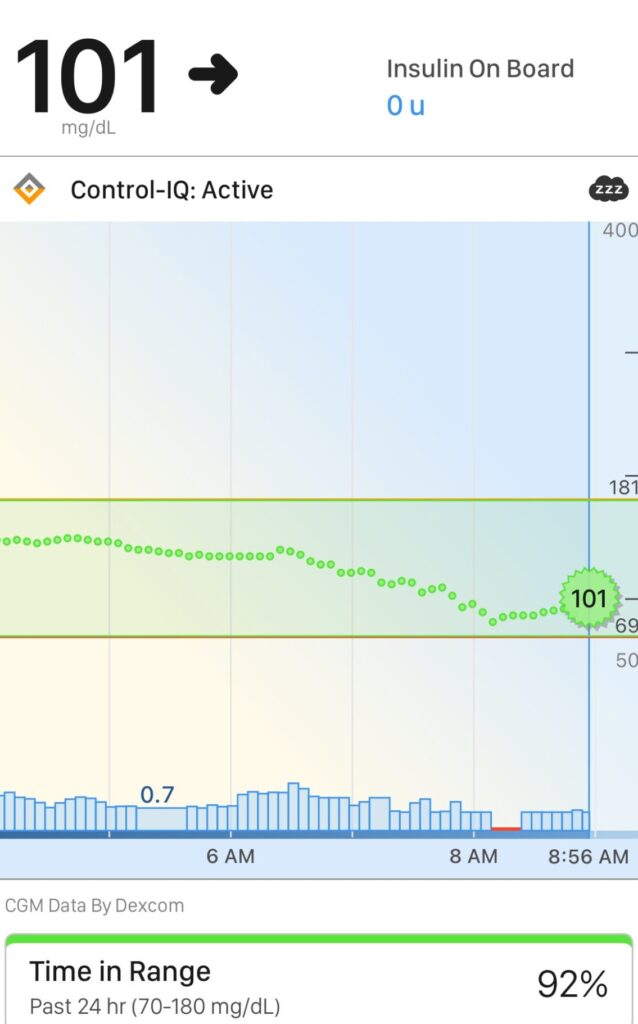
The result was that I brought my time in range back to over ninety-two percent simply by reducing total fat intake earlier in the day.
How Fat Can Affect Blood Sugar and Insulin Sensitivity
Most people understand that carbohydrates raise blood sugar. But fat has a more subtle, delayed effect that is often overlooked.
Dietary Fat and Insulin Resistance
Dietary fat slows gastric emptying, which might seem helpful at first because slower digestion can mean slower glucose absorption. But consuming large amounts of fat over the course of a day can temporarily impair insulin sensitivity. Essentially, the insulin you take does not work as efficiently to move glucose into cells. Medical and metabolic research sometimes refers to this as lipotoxicity, a condition in which excess fat interferes with insulin signaling.
Even if you take the right insulin dose for a meal, your body may not respond normally. Blood sugar rises and stays elevated for hours. This is not a pump or insulin problem. It is a physiological response to high fat intake combined with carbohydrates.
Fat Density and Energy Overload
High-fat foods such as cheese, creams, cheesy sauces, or high-fat meats like bacon and sausage are dense in saturated fat. When high-fat volume is present in the bloodstream after meals, cells, particularly in muscles and the liver, become less responsive to insulin. This temporary insulin resistance explains why glucose can remain elevated for hours and why later, once enough insulin finally works, the drop can feel extreme.
My Experience With Fat-Induced Insulin Resistance
On that high-fat day, my meals were:
Breakfast: cheese and nuts
Lunch: chicken, feta cheese, nuts and olives
Snacks: sausage and nuts
Dinner: vegetable pasta with fruit
Despite taking my normal insulin dose for the carbohydrates at dinner, my blood sugar remained elevated for six hours. Only after a long delay did it drop, and it was a dramatic drop at 2 a.m.
Using the same infusion set for another day confirmed that it was not a device issue. The problem was the fat intake interacting with the carbohydrate meal.
After reducing my fat intake and spreading it more evenly throughout the day, my glucose control returned to normal. My time in range increased to over ninety-two percent. This was real, measurable feedback that the fat was the culprit.
Understanding Carbohydrates and Insulin
Even though fat caused my most dramatic blood sugar disruption, carbohydrates are still a primary driver of glucose.
Why Carbs Spike Insulin
Carbohydrates are broken down into glucose.
Glucose enters the blood, prompting insulin release from the pancreas.
Insulin moves glucose into cells for energy or storage.
Chronically high insulin without energy use can lead to glucose being stored as fat, which makes weight management harder.
Why Carbs Can Be Addictive
Frequent carbohydrate intake reinforces cravings. When insulin lowers blood sugar quickly, it triggers hunger, which leads to more carbohydrate consumption.
Stress and anxiety can intensify carb cravings because the brain seeks quick energy and dopamine reward.
How to Balance Carbs Without Feeling Deprived
Distribute carbohydrates around physical activity. Muscles use glucose more efficiently during and after exercise.
Combine carbohydrates with protein and some fat to slow absorption, reduce spikes, and increase satiety.
Choose fiber-rich, low-glycemic carbohydrates such as lentils, chickpeas, vegetables, and small portions of sweet potato.
Moderate intake rather than eliminating carbohydrates entirely. Match intake to energy needs and activity.
Practical Strategies for Managing Dietary Fat and Blood Sugar
Track total fat intake. Be mindful of fat consumption across the day, not just per meal. High fat early can impair insulin sensitivity later. My personal goal is less than twenty grams per meal for most meals.
Balance fat, carbohydrates, and protein. Limit heavy-fat meals immediately before or after carbohydrate-heavy meals. Balanced meals help stabilize blood sugar.
Spread fat intake. Enjoy fat-rich foods in moderation and space them out throughout the day, especially if you eat a moderate- to high-carb diet.
Time carbohydrates around activity. Carbohydrates are used more efficiently when muscles are active. Plan carb intake before or after workouts for better insulin sensitivity.
Monitor patterns and time in range. Use your continuous glucose monitor and time in range data to guide decisions. Your body gives you clear signals about what works.
Real-World Meal and Snack Ideas for Stable Blood Sugar
Breakfast Ideas
Greek yogurt with berries and a tablespoon of granola or nuts
Egg scramble with vegetables and a slice of low-glycemic sprouted bread
Low-fat cottage cheese with berries and a sprinkle of flax or chia seeds
Lunch Ideas
Grilled chicken or turkey with roasted non-starchy vegetables and a small portion of lentils or chickpeas
Salad with leafy greens, canned tuna or salmon, beans, and one to two tablespoons of mashed avocado
Turkey or chicken lettuce wraps with cucumber, a little feta cheese, and a side of roasted sweet potato
Dinner Ideas
Baked fish or chicken with roasted cauliflower, broccoli, or zucchini and black beans
Stir-fried tofu or tempeh with non-starchy vegetables and a handful of edamame
Omelet with spinach, mushrooms, and a side of roasted vegetables or a few slices of sweet potato
Snack Ideas
Hard-boiled eggs with cucumber slices or cherry tomatoes
Protein shake with unsweetened plant milk and low-glycemic fruit like berries
Edamame or roasted chickpeas
Celery or bell pepper sticks with a small amount of nut butter
Vanilla Greek yogurt with PB Fit mixed in, plus carrots or apple slices
The key is protein to improve insulin efficiency, moderate low-glycemic carbohydrates to stabilize blood sugar, and keeping fat moderate to avoid blunting insulin action.
What This Means for People With Diabetes
Many people are surprised by unexplained insulin resistance. We often assume high blood sugar after a meal is due to too many carbohydrates or not enough insulin. But dietary fat can blunt insulin action for hours, making doses less effective.
It might not be your infusion set, your insulin, or your timing. It could be what you ate earlier. Paying attention to all macronutrients and using glucose data to inform decisions gives you more control and fewer surprises.
Final Thoughts
Diabetes management is complex. Insulin, activity, stress, sleep, and food all play a role. While carbohydrates get most of the attention, total dietary fat and how it is distributed throughout the day can have a major impact on blood sugar and insulin sensitivity.
Even after decades of experience, my body still teaches me lessons. By paying attention to fat as well as carbohydrates, I improved my time in range and avoided the terrifying blood sugar rollercoaster of insulin resistance.
Look at your patterns. What happens on days with very high fat? How does that compare with days with balanced fat intake? Your glucose data can help answer those questions and make diabetes management much more manageable.

Schedule with Ariel Warren – Take Control of Your Diabetes and Your Life
Schedule a personalized consultation with Ariel Warren, Registered Dietitian and Certified Diabetes Educator, living with Type 1 Diabetes since 1995. Ariel specializes in insulin pumps, advanced diabetes management, nutrition, exercise, and weight loss.
We work through secure video calls, making it convenient to get expert guidance from home. Many insurance plans cover our visits. Usually just a copay or completely free!
Ariel will help you create a customized plan to stabilize your blood sugar, optimize insulin use, improve your metabolism, and reach your health and weight goals with diabetes.
Take control of your diabetes and live your best life. Book your appointment with Ariel today!